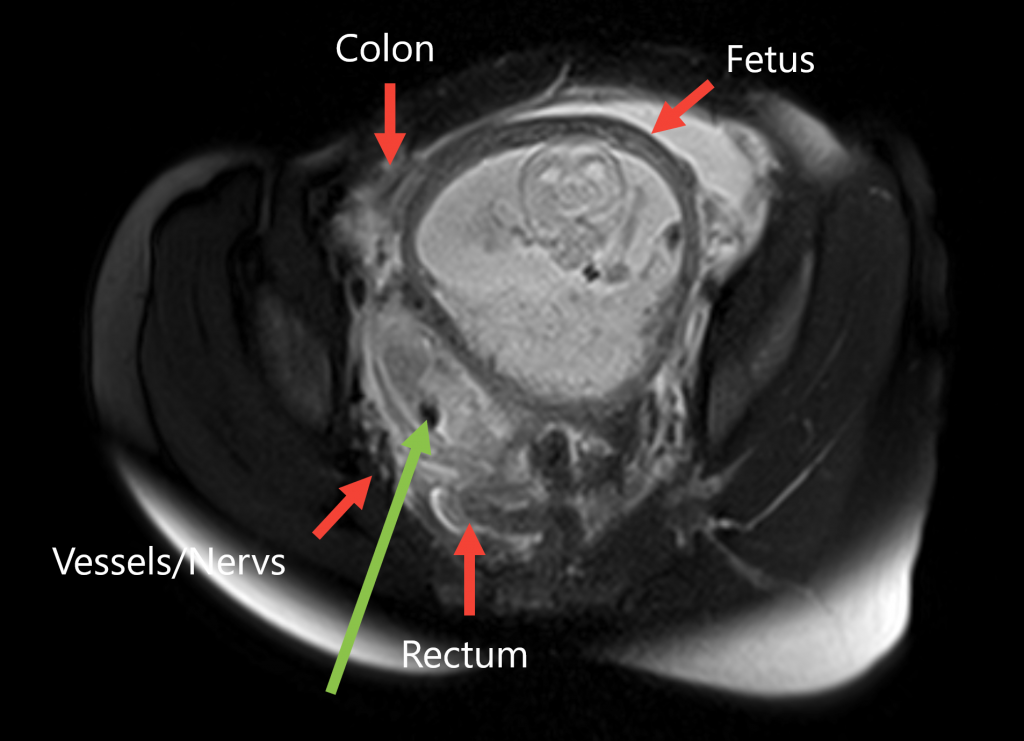
MRI (Magnetic Resonance Imaging) offers a multitude of advantages that have established it as a pivotal tool in modern medicine. Firstly, MRI is a non-invasive imaging technique, eliminating the need for harmful ionizing radiation present in other imaging methods. This makes it safe for patients of all ages, including children and pregnant women. Additionally, MRI provides exceptional soft tissue contrast, allowing for the clear visualization of various structures within the body, including the brain, spinal cord, organs, and joints. Its high-resolution images aid in the early detection and accurate diagnosis of a wide range of conditions. With its exceptional capabilities, MRI continues to play an integral role in advancing medical knowledge, guiding treatment decisions, and enhancing patient care.
Our group uses MRI for different types of interventions, such as:

MR-guided Percutaneous Ablation

Unlike ultrasound and CT, MRI can visualize lesions that would otherwise remain undetected due to its excellent soft-tissue contrast. In addition, MRI allows temperature measurement, which is extremely useful in tumor ablation procedures, as it enables monitoring of the progress and completeness of the ablation. Furthermore, unlike CT, MRI does not involve ionizing radiation.
The high flexibility in positioning and acquiring 2D planes and 3D volumes in space enables real-time intervention paths at virtually any angle. With appropriate techniques, interactive adjustment of imaging planes is also possible. This allows even difficult-to-localize and hard-to-reach tumors—such as lesions in the hepatic dome near the diaphragm—to be targeted under free breathing conditions. As a result, MRI-guided interventions can reduce risk, lower recurrence rates, and shorten hospital stays compared to surgery, particularly in tumor ablation.
For these reasons, interventional MRI (iMRI) is a key research focus at our institute and is also used in clinical care. In addition to diagnostic biopsies (e.g., in the liver, kidneys, or extremities), we perform minimally invasive cortisone and Botox injections as well as microwave ablations.
During ablation, pencil-lead–thin applicators are positioned minimally invasively into the tumor using real-time MRI guidance. The tissue is then locally heated to temperatures of up to 120 °C, causing tumor cell death. This process is monitored using MRI-based thermometry. Follow-up imaging is performed two months after ablation and then every six months to assess treatment success and detect new tumors at an early stage.


MR-guided Pain Management
The piriformis muscle is a gluteal muscle that, due to causes such as muscle tension or shortening, can exert pressure on the adjacent sciatic nerve. This results in a compression syndrome, which presents with typical sciatica symptoms, including radiating pain into the buttock and leg.
In severe, chronic cases, MRI-guided injection of botulinum toxin A (Botox®) into the piriformis muscle is a minimally invasive, image-guided treatment option [4][5]. The neurotoxin blocks signal transmission from nerves to the muscle, leading to temporary denervation and weakening of the muscle. Pain relief is achieved through reduced muscle tone, and the decreased muscle volume also relieves pressure on the neighboring sciatic nerve, resolving the compression.
A key advantage of MRI-guided injection is that both the needle and the muscle can be visualized, allowing very precise delivery of botulinum toxin into the affected muscle. This significantly improves safety and effectiveness. In addition, the painful sciatic nerve can be temporarily anesthetized along its course below the piriformis muscle (in the infrapiriform foramen) by injecting long-acting local anesthetics and corticosteroids. This is often helpful in breaking acute pain cycles.
At the Institute of Diagnostic and Interventional Radiology, this procedure is used both clinically and in research to further refine and evaluate the technique. We work closely with the Department of Rehabilitation Medicine at Hannover Medical School (MHH), which thoroughly evaluates patients and excludes other causes of symptoms.

MR-guided Biopsy
Histological examination of tissue samples is often crucial for the reliable diagnosis of tumors or inflammatory changes. In some cases, however, suspicious tissue structures are only visible—or best visualized—on magnetic resonance imaging (MRI) and are difficult to localize using other imaging modalities.
In MRI-guided biopsy, a fine biopsy needle is precisely advanced into the suspicious lesion under direct MRI guidance [6][7]. The excellent soft-tissue contrast of MRI allows very accurate visualization of both the target structure and the surrounding anatomy, enabling precise needle placement and the collection of representative tissue samples.
Another advantage of MRI is that it does not use ionizing radiation and allows flexible acquisition of 2D slices and 3D volumes in arbitrary planes. This makes it possible to plan and adjust even complex needle trajectories during the procedure.
At the Institute of Diagnostic and Interventional Radiology, MRI-guided biopsy is primarily used for lesions that are difficult to access or only visible on MRI, for example in the liver, kidneys, muscles, or soft tissues of the extremities. The precise image guidance improves diagnostic accuracy while reducing the risk of complications.

Lymphangiography
The lymphatic system plays a central role in the transport of tissue fluid, fats, and immune cells throughout the body. Disorders of this system can lead to leakage of lymph fluid (lymphatic leakage) or impaired lymph drainage. Such complications may occur, for example, after surgery, in tumor diseases, or due to congenital malformations, and may manifest as chylothorax, lymphatic fistulas, or persistent lymph collections.
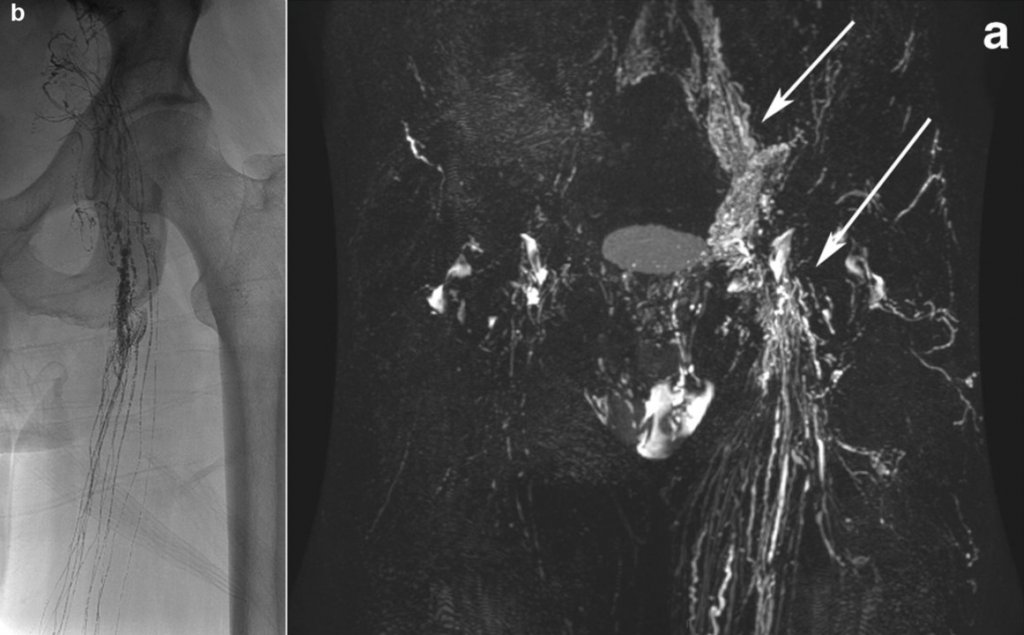
Lymphangiography is a minimally invasive imaging procedure used to visualize the lymphatic system [8][9]. In this procedure, fine lymphatic vessels—usually in the region of the dorsum of the foot or the groin—are punctured, and a contrast agent is introduced into the lymphatic system. The lymphatic vessels and potential leakages can then be visualized using MRI.
In addition to its diagnostic role, lymphangiography can often be directly combined with interventional therapy. Leaking lymphatic vessels can be selectively sealed, and pathological lymphatic connections can be treated. In many cases, this allows surgical treatment to be avoided.
At the Institute of Diagnostic and Interventional Radiology, lymphangiography is used both for precise diagnosis of complex lymphatic disorders and for minimally invasive treatment of lymphatic leakages. Modern image-guided techniques enable visualization and targeted treatment of even very small lymphatic vessels.
Abscess Drainage
An abscess is a localized, encapsulated collection of pus that can develop as a result of infection. Such accumulations can occur in the abdominal cavity, within organs, or in soft tissue and may cause severe pain, fever, and significant impairment of the patient’s general condition.
Percutaneous abscess drainage is a minimally invasive procedure used to treat such infections [10][11]. Under imaging guidance—typically using ultrasound, CT, or MRI—a thin drainage catheter is inserted into the abscess through a small skin puncture. The pus can then be continuously drained through this catheter, reducing pressure within the abscess and allowing the infection to heal.
Image-guided drainage enables very precise catheter placement while sparing surrounding structures. In many cases, this can avoid the need for major surgery or at least significantly reduce its extent. The procedure is often combined with antibiotic therapy.
At the Institute of Diagnostic and Interventional Radiology, abscess drainages are routinely performed using modern image guidance. The minimally invasive approach often allows patients to stabilize and recover more quickly, which can also shorten hospital stays.
References:
[1] Hille et al. A novel tool for monitoring and assessing the outcome of thermal ablations of hepatic lesions. Current Directions in Biomedical Engineering 7 1 (2021).
[2] Ahmed et al. Image-guided tumor ablation: standardization of terminology and reporting criteria. Radiology (2014).
[3] Hinshaw et al. Percutaneous tumor ablation tools: microwave, radiofrequency, or cryoablation—what should you use and why? Radiographics (2014).
[4] Yan et al. Piriformis syndrome: pain response outcomes following CT-guided injection and incremental value of botulinum toxin injection. Diagnostic and Interventional Radiology (2021).
[5] Childers et al. Botulinum toxin type A use in piriformis muscle syndrome: a pilot study. American Journal of Physical Medicine & Rehabilitation (2002).
[6] Stattaus et al. MR-guided liver biopsy within a short, wide-bore 1.5 Tesla MR system. European Radiology (2008).
[7] Schmidt et al. Diagnostic yield of MR-guided liver biopsies compared with CT- and US-guided biopsies. Journal of Vascular and Interventional Radiology (1999).
[8] Nadolski et al. Feasibility of ultrasound-guided intranodal lymphangiography for thoracic duct embolization. Journal of Vascular and Interventional Radiology (2012).
[9] Itkin et al. Modern techniques of lymphangiography and interventions: current status and future development. Cardiovascular Interventional Radiology (2018).
[10] vanSonnenberg et al. Percutaneous abscess drainage: update. World Journal of Surgery (2001).
[11] Lorenz et al. Complications of percutaneous fluid drainage. Seminars in Interventional Radiology (2006).

